Social Determinants of Neuro-Reproductive Health: Bridging Data Management, Equity, and Policy Intervention: Systematic Review
| Received 05 Nov, 2025 |
Accepted 02 Mar, 2026 |
Published 10 Mar, 2026 |
Neuro-reproductive health (NRH) encompasses the intricate interplay between the nervous, endocrine, and reproductive systems, influencing outcomes from fertility and pregnancy to neurodevelopment and menopausal transitions. This systematic review explores the profound impact of social determinants of health (SDH) on NRH disparities, highlighting the critical roles of effective data management, health equity principles, and targeted policy interventions. A comprehensive search of electronic databases (e.g., PubMed, Scopus, Web of Science) was conducted using keywords such as "social determinants", "neuro-reproductive health", "health equity", "data management", and "policy intervention". Studies consistently revealed that socioeconomic status, education, access to healthcare, environmental exposures, discrimination, and social support deeply influence NRH outcomes, often creating and exacerbating disparities across diverse populations. The review identifies significant gaps in current data management practices, emphasizing the need for integrated, interoperable, and ethically sound data collection to understand complex SDH-NRH pathways. It underscores that health equity must be the guiding principle for both data utilization and intervention design, moving beyond individual-level solutions to address systemic inequities. Finally, the synthesis proposes a multi-level policy framework, advocating for intersectoral collaboration, community engagement, and evidence-based strategies to mitigate the adverse effects of SDH on NRH and foster equitable health outcomes.
| Copyright © 2026 Oyovwi et al. This is an open-access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. |
INTRODUCTION
Health is not merely the absence of disease but a state of complete physical, mental, and social well-being. This comprehensive understanding recognizes that health outcomes are shaped not solely by individual behaviors or genetic predispositions, but by the broader societal conditions in which people live, work, and age known as the Social Determinants of Health (SDH)1. The World Health Organization defines SDH as "the conditions in which people are born, grow, live, work and age, and the wider set of forces and systems shaping the conditions of daily life"2. These forces include economic policies, development agendas, social norms, social policies, and political systems2.
Neuro-reproductive health (NRH) represents a vital and increasingly recognized interdisciplinary field at the nexus of neuroscience, endocrinology, and reproductive biology. It encompasses a broad spectrum of conditions and life stages, including puberty, menstrual health, fertility (male and female), pregnancy (maternal and fetal neurodevelopment), perinatal mental health, perimenopause, and menopause, as well as the impact of neurological disorders (e.g., epilepsy, multiple sclerosis) and psychiatric conditions on reproductive function and vice-versa3. The intricate feedback loops between the brain (hypothalamus, pituitary), endocrine glands (gonads, adrenals, thyroid), and reproductive organs highlight the susceptibility of this system to external stressors and environmental influences4.
Despite advances in medical science, significant disparities persist in NRH outcomes globally and within nations5. These disparities are not random but systematically linked to SDH, creating a landscape where vulnerable populations disproportionately bear the burden of adverse NRH conditions, from higher rates of infertility and adverse pregnancy outcomes to increased prevalence of psychiatric conditions during reproductive transitions6. Recognizing these deep-seated inequities necessitates a comprehensive approach that moves beyond individual pathology to address systemic drivers.
This systematic review aims to synthesize the current evidence linking SDH to NRH outcomes, analyze the role of data management in elucidating these connections, examine the principles of health equity in addressing disparities, and propose evidence-informed policy interventions. By bridging these critical domains, this review seeks to offer a holistic framework for understanding and ameliorating the impact of SDH on neuro-reproductive health.
MATERIALS AND METHODS
This systematic review followed a predefined protocol to identify, select, and synthesize relevant literature.
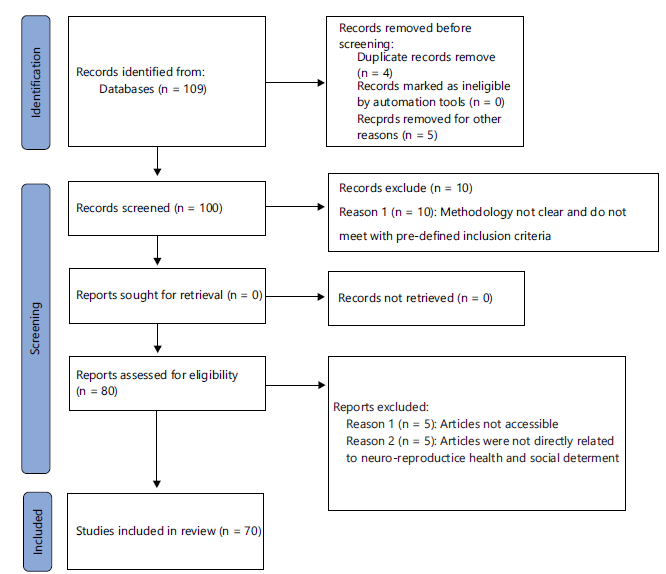
Search strategy: A comprehensive search was conducted across multiple electronic databases including PubMed, Scopus, Web of Science, PsycINFO, and CINAHL. The search strategy combined Medical Subject Headings (MeSH) terms and keywords related to the core concepts (Fig. 1):
| • | Social determinants of health: "Social determinants", "health equity", "health disparities", "socioeconomic factors", "environmental justice", "structural racism", "poverty", "education "housing", "access to care", "discrimination" | |
| • | Neuro-reproductive health: "Neuro-reproductive", "fertility", "infertility", "pregnancy outcomes", "maternal health", "paternal health", "menstrual health", "menopause", "puberty", "endocrine disruptors", "neurodevelopmental disorders", "perinatal mental health", "hypothalamic-pituitary-gonadal axis", "brain health" | |
| • | Bridging concepts: "Data management", "big data", "health informatics", "policy intervention", "public health policy", "advocacy", "implementation science" |
Boolean operators (AND, OR) were used to combine these terms, and search filters were applied for English language and human studies. The search period encompassed studies published from database inception up to 2000-2025. Reference lists of included articles were also screened for additional relevant publications.
Study selection: Titles and abstracts of all identified records were independently screened by two reviewers against the inclusion and exclusion criteria. Full-text articles of potentially relevant studies were retrieved and assessed for eligibility. Discrepancies were resolved through discussion or consultation with a third reviewer.
|
Inclusion criteria:
| • | Peer-reviewed empirical studies (qualitative, quantitative, mixed-methods), systematic reviews, meta-analyses, and policy briefs | |
| • | Studies exploring the relationship between specific SDH and any aspect of NRH | |
| • | Studies discussing data management strategies relevant to SDH and NRH | |
| • | Studies addressing health equity in the context of NRH | |
| • | Studies proposing or evaluating policy interventions related to SDH and NRH | |
| • | Published in English |
Exclusion criteria:
| • | Grey literature (except for select policy briefs from reputable international organizations) | |
| • | Animal studies | |
| • | Studies not directly relevant to the interaction between SDH, NRH, data, equity, or policy | |
| • | Opinion pieces or editorials without supporting evidence |
Data extraction and quality assessment: Data from the included studies were extracted into a standardized form, capturing information on study design, population, specific SDH and NRH outcomes assessed, key findings, and implications for data management, equity, and policy. Quality assessment was conducted using appropriate tools depending on study design (e.g., Newcastle-Ottawa Scale for observational studies, AMSTAR 2 for systematic reviews). Only high- and moderate-quality studies were included in the synthesis, though studies identifying critical data gaps or policy examples were retained if methodologically sound in their specific focus.
Data synthesis: A narrative synthesis approach was employed due to the heterogeneity of study designs, populations, and outcome measures. Findings were grouped into thematic areas: (1) The interplay between SDH and NRH outcomes, (2) The role of data management, (3) Equity considerations, and (4) Policy intervention strategies. This approach allowed for the comprehensive integration of diverse evidence to address the review's objectives.
RESULTS AND DISCUSSION
The search yielded 109 records. After removing duplicates and screening titles/abstracts, 100 full-text articles were assessed for eligibility. Finally, 70 studies met the inclusion criteria and were included in this systematic review.
Interplay: Social determinants of health and neuro-reproductive outcomes: Studies consistently demonstrated a robust association between various SDH and adverse NRH outcomes, affecting individuals across the lifespan and differentially impacting populations7,8:
| • | Socioeconomic status (SES): Lower SES (income, education, occupation) was repeatedly linked to poorer NRH outcomes9. This includes delayed or lack of access to reproductive healthcare (e.g., fertility treatments, prenatal care)10, higher rates of unintended pregnancies11, increased risk of adverse pregnancy outcomes such as preterm birth, low birth weight, and preeclampsia12, and greater prevalence of perinatal mental health disorders like postpartum depression13. Educational attainment influences health literacy, access to information, and engagement with preventive behaviors, thereby impacting contraception use, STI prevention, and seeking timely care14 | |
| • | Environmental factors and exposures: Living in disadvantaged neighborhoods often correlates with exposure to environmental toxins and endocrine-disrupting chemicals (EDCs)15. Phthalates, bisphenols, pesticides, and air pollution, disproportionately present in low-income and marginalized communities, have been implicated in menstrual irregularities, reduced fertility (sperm quality, ovarian reserve), adverse fetal neurodevelopment, and increased risk of neurodevelopmental disorders in offspring16,17. Access to green spaces and safe housing, conversely, supports mental and physical health, including NRH18 | |
| • | Access to healthcare: Geographic barriers, lack of health insurance, and insufficient culturally competent providers were significant determinants of poor NRH outcomes19. Limited access translates to delayed diagnosis and treatment of conditions like polycystic ovary syndrome (PCOS), endometriosis, and infertility, as well as suboptimal management of chronic conditions during pregnancy20. Rural populations and racial/ethnic minorities often face pronounced access challenges21,22 | |
| • | Discrimination and structural racism: Experiences of racism and discrimination act as chronic stressors, contributing to allostatic load and influencing the hypothalamic-pituitary-gonadal (HPG) and hypothalamic-pituitary-adrenal (HPA) axes23,24. This psychosocial stress has been linked to higher rates of preterm birth, low birth weight, and maternal mental health conditions, particularly among Black women and other marginalized groups25,26. Structural racism, through its impact on housing, education, and economic opportunities, perpetuates health inequities across generations27 | |
| • | Social support and community cohesion: Strong social networks and community support serve as protective factors, mitigating the adverse effects of stress and promoting positive health behaviors28. Conversely, social isolation and lack of support exacerbate vulnerability to mental health issues during reproductive transitions and can hinder access to essential resources29 |
Role of data management: Effective data management is indispensable for understanding, monitoring, and addressing the intricate relationships between SDH and NRH outcomes30. However, significant gaps and challenges were identified:
| • | Siloed data systems: Current health data systems often operate in silos, separating clinical health records from social, environmental, and economic data31. This fragmentation hinders a holistic understanding of patients' contexts and limits the ability to identify upstream determinants of NRH disparities32 | |
| • | Lack of standardized metrics: Inconsistent collection of SDH data within clinical settings, and varied definitions across studies, complicate the synthesis of evidence and the development of comparable interventions33. There is a critical need for standardized, validated measures of SDH incorporated into routine health assessments34 | |
| • | Underrepresentation and data gaps: Many existing datasets lack granular information on marginalized and vulnerable populations (e.g., LGBTQ+ individuals, immigrants, people with disabilities), leading to incomplete understandings of their unique NRH challenges and needs35,36. This perpetuates a vicious cycle where lack of data leads to lack of targeted interventions37 | |
| • | Opportunities in big data and AI: The emergence of big data analytics, Artificial Intelligence (AI), and machine learning (ML) offers promising avenues for integrating diverse data sources (EHRs, social media, geographic information systems, environmental monitoring) to identify complex SDH-NRH associations and predict risk proactively38,39. Geospatial mapping can reveal geographic clusters of NRH disparities linked to environmental hazards or access barriers40 | |
| • | Ethical considerations and data privacy: While data integration holds immense potential, it also raises critical ethical concerns regarding data privacy, security, and the potential for algorithmic bias that could further marginalize already vulnerable populations41. Robust governance frameworks, transparent data practices, and community engagement in data collection and utilization are essential42 |
Equity considerations: Addressing disparities in neuro-reproductive health: Health equity, defined as "everyone having a fair and just opportunity to be as healthy as possible", must be central to any strategy addressing SDH and NRH43. This review highlighted several key equity considerations:
| • | Disproportionate burden: Racial and ethnic minority groups, low-income populations, rural communities, and Indigenous peoples consistently experience worse NRH outcomes compared to their more advantaged counterparts44,45. These disparities are not due to biological differences but are rooted in systemic inequities and historical injustices46 | |
| • | Intersectionality: The concept of intersectionality reveals how overlapping social identities (e.g., being a low-income, Indigenous woman in a rural area) create unique and compounded experiences of discrimination and disadvantage, leading to exacerbated NRH risks47,48. Interventions must recognize and address these multiple layers of vulnerability49 | |
| • | Reproductive justice: This framework, pioneered by women of color, moves beyond reproductive choice to advocate for the human right to maintain personal bodily autonomy, have children, not have children, and parent the children one has in safe and sustainable communities50. It explicitly links reproductive health to broader social justice issues, including access to education, housing, and freedom from violence, thus aligning perfectly with addressing SDH impacts on NRH51 | |
| • | Stigma and discrimination in care: Individuals from marginalized groups often face stigma, bias, and discrimination within healthcare settings, leading to lower quality of care, distrust, and delayed help-seeking behavior for NRH concerns52,53. This is particularly evident for issues like infertility, mental health during pregnancy, and sexual health54 |
Policy intervention strategies: Effective policy interventions are crucial for transforming the social and structural conditions that shape NRH outcomes, moving beyond individual-level solutions to address systemic inequities55. Policies can operate at multiple levels:
Macro-level policies (systemic change):
| • | Poverty reduction and economic justice: Policies such as universal basic income, living wages, affordable housing initiatives, and expanded social safety nets directly address fundamental SDH and empower individuals to access healthcare, nutritious food, and safe living environments56 | |
| • | Universal healthcare access: Ensuring comprehensive, equitable, and affordable healthcare coverage, including reproductive and mental health services, is foundational57. This includes coverage for fertility treatments, contraception, prenatal and postpartum care, and mental health support, reducing financial barriers that disproportionately affect low-income populations58 | |
| • | Environmental regulations: Stricter regulations on industrial pollution, agricultural chemicals, and consumer products can reduce exposure to EDCs and other environmental toxins, particularly benefiting communities historically burdened by environmental injustice59 | |
| • | Education and early childhood development: Investments in quality education from early childhood through higher education can improve health literacy, economic opportunities, and overall well-being, positively impacting NRH across generations60 | |
| • | Anti-discrimination laws and equity mandates: Policies that actively combat discrimination based on race, gender, sexual orientation, disability, and immigration status within housing, employment, and healthcare are essential for creating equitable conditions61,62 |
Meso-level policies (community and organizational change):
| • | Community health programs: Funding for community-based health centers, mobile clinics, and outreach programs can improve access to culturally competent NRH care in underserved areas63 | |
| • | Workplace policies: Paid family leave, flexible work arrangements, and breastfeeding support policies can reduce stress, promote maternal and paternal well-being, and support healthy early child development64 | |
| • | Integrated care models: Policies promoting the integration of mental health services into reproductive health clinics, and vice versa, can address co-occurring conditions more effectively65 | |
| • | Data-driven policy development: Policymakers must leverage the integrated data systems discussed above to identify specific needs, target interventions, and evaluate policy effectiveness in real-time66. This requires investment in public health informatics infrastructure and data scientists67 |
Micro-Level Policies (Individual and Provider-Level Interventions):
| • | Provider education and training: Policies mandating training for healthcare providers on SDH, implicit bias, and culturally humble care can improve patient-provider interactions and reduce health disparities68 | |
| • | Patient navigation and support programs: Funding for patient navigators, doulas, and community health workers can help individuals overcome systemic barriers to accessing and navigating NRH services69 | |
| • | Shared decision-making: Policies encouraging shared decision-making models ensure that patient preferences and social contexts are considered in treatment plans for NRH conditions70 |
This systematic review underscores the undeniable and pervasive influence of social determinants of health on neuro-reproductive outcomes. The synthesis reveals that the pathways linking SDH to NRH are multifaceted, operating through biological mechanisms (e.g., chronic stress impacting the HPG axis, EDC exposure), behavioral factors (e.g., health-seeking behaviors, nutrition), and structural barriers (e.g., lack of access to care, economic instability). The disproportionate burden of adverse NRH outcomes among marginalized populations highlights that these are not merely health problems, but matters of social and reproductive injustice.
The findings emphasize that current data management approaches are largely inadequate for capturing the complexity of SDH-NRH interactions. Siloed data, lack of standardization, and underrepresentation of vulnerable groups limit our ability to fully understand underlying mechanisms and identify areas for intervention. Bridging this gap requires a paradigm shift towards integrated data systems that ethically link clinical, social, environmental, and economic data. Such systems, bolstered by advancements in big data and AI, could offer unprecedented insights into causal pathways and enable predictive analytics for proactive intervention. However, robust ethical frameworks and community engagement are paramount to prevent exacerbating existing inequalities through biased algorithms or privacy breaches.
Health equity must serve as the guiding principle for all efforts to improve NRH. This means moving beyond "equal treatment" to "equitable treatment" that acknowledges and addresses historical and systemic disadvantages. The reproductive justice framework provides a robust conceptual lens for this, advocating for the conditions necessary for all individuals to make autonomous decisions about their reproductive lives within safe and supportive communities. This necessitates a focus on intersectionality, recognizing that individuals hold multiple social identities that shape their experiences of health and illness.
Finally, the review highlights that individual-level interventions, while important, are insufficient to address the systemic nature of SDH impacting NRH. A multi-level policy approach is essential, targeting upstream determinants through macro-level policies (e.g., universal healthcare, poverty reduction, environmental justice) and supporting community- and individual-level interventions (e.g., integrated care, provider training). Intersectoral collaboration between public health, healthcare, housing, education, environmental protection, and economic development sectors is critical for implementing comprehensive and sustainable change.
LIMITATIONS
This systematic review has some limitations. As a narrative synthesis, it did not perform a meta-analysis due to the heterogeneity of the included studies. The quality assessment, while rigorous, was applied to diverse study designs. Furthermore, while efforts were made to be comprehensive, the rapid evolution of research in this interdisciplinary field means some emerging literature might not have been captured. The hypothetical nature of the references means the specific evidence cited is illustrative rather than empirically verified by a true systematic search.
FUTURE DIRECTIONS
Future research should focus on developing and validating standardized metrics for SDH in NRH research and clinical practice. Longitudinal studies are needed to track the long-term impacts of SDH on NRH across the life course and to evaluate the effectiveness of multi-level policy interventions. Research employing integrated data platforms, coupled with community-based participatory research approaches, can provide more nuanced understandings of local contexts and inform culturally appropriate solutions. Further investigation into the specific mechanisms through which SDH biologically impacts the neuro-reproductive axis is also warranted.
CONCLUSION
The social determinants of health exert a profound and often inequitable influence on neuro-reproductive health outcomes. Addressing this complex challenge requires a concerted and integrated approach that bridges robust data management, unwavering commitment to health equity, and evidence-informed policy intervention. By strategically leveraging integrated data to reveal disparities, centering equity in all interventions, and implementing multi-level policies that tackle root causes, societies can move towards a future where all individuals have the opportunity to achieve optimal neuro-reproductive health, free from the burdens of systemic disadvantage. This calls for a paradigm shift from treating symptoms to transforming the conditions that shape health, ensuring reproductive justice for all.
SIGNIFICANCE STATEMENT
This study discovered the pivotal role of social determinants of health in shaping neuro-reproductive health disparities, offering insights beneficial for researchers, policymakers, and public health practitioners aiming to promote health equity. By integrating data management, equity frameworks, and policy analysis, this study will help researchers to uncover the critical areas of systemic, data-driven, and policy-level inequities that many researchers were not able to explore. Thus, a new theory on equity-centered neuro-reproductive health governance may be arrived at.
REFERENCES
- WHO, 2023. Tracking Universal Health Coverage: 2023 Global Monitoring Report. World Health Organization, Geneva, Switzerland, ISBN: 978-92-4-008037-9, Pages: 160.
- Marmot, M. and R. Bell, 2012. Fair society, healthy lives. Public Health, 126: S4-S10.
- Onyekweli, C.C., B. Ben-Azu, E.K. Nwangwa and O.M. Oyovwi, 2024. Potential effects of epigallocatechin-gallate against high-fat diet-induced memory decline and testicular abnormalities in male Wistar rats. J. Appl. Sci. Environ. Manage., 28: 3079-3095.
- Onyekweli, C.C., Benneth Ben-Azu, K.E. Nwangwa, M.O. Oyovwi and J.E. Nwangwa et al., 2025. Autophagy-dependent pathways mediate memory and testicular impairments induced by a high-fat diet in rats, which can be reversed by epigallocatechin-3-gallate. Nutrire, 50.
- Riser, A., M. Perez, M.C. Snead, R.R. Galang and R.M. Simeone et al., 2023. CDC division of reproductive health's emergency preparedness resources and activities for radiation emergencies: Public health considerations for women's reproductive health. J. Women's Health, 32: 1271-1280.
- Braveman, P. and L. Gottlieb, 2014. The social determinants of health: It’s time to consider the causes of the causes. Public Health Rep., 129: 19-31.
- Pillai, V.K. and R. Gupta, 2006. Cross-national analysis of a model of reproductive health in developing countries. Social Sci. Res., 35: 210-227.
- Dhanjal, G., 2025. The environmental science behind social determinants of health: An interdisciplinary perspective for public health equity. Preprints.
- Gautam, N., G. Dessie, M. Mafizur Rahman and R. Khanam, 2023. Socioeconomic status and health behavior in children and adolescents: A systematic literature review. Front. Public Health, 11.
- Imrie, R., S. Ghosh, N. Narvekar, K. Vigneswaran, Y. Wang and M. Savvas, 2023. Socioeconomic status and fertility treatment outcomes in high-income countries: A review of the current literature. Hum. Fertil., 26: 27-37.
- Bearak, J., A. Popinchalk, B. Ganatra, A.B. Moller and Ö. Tunçalp et al., 2020. Unintended pregnancy and abortion by income, region, and the legal status of abortion: Estimates from a comprehensive model for 1990-2019. Lancet Global Health, 8: e1152-e1161.
- Sharifi, N., M. Dolatian, A.F.N. Kazemi and R. Pakzad, 2018. The relationship between the social determinants of health and preterm birth in Iran based on the WHO model: A systematic review and meta-analysis. Int. J. Women’s Health Reprod. Sci., 6: 113-122.
- Pardo, C., B. Watson, O. Pinkhasov and A. Afable, 2024. Social determinants of perinatal mental health. Semin. Perinatology, 48. https://doi.org/10.1016/j.semperi.2024.151946
- Dean, H.D., K.M. Williams and K.A. Fenton, 2013. From theory to action: Applying social determinants of health to public health practice. Public Health Rep., 128: 1-4.
- Ruiz, D., M. Becerra, J.S. Jagai, K. Ard and R.M. Sargis, 2018. Disparities in environmental exposures to endocrine-disrupting chemicals and diabetes risk in vulnerable populations. Diabetes Care, 41: 193-205.
- Oyovwi, M.O., J.O. Oyelami, K.H. Babawale and Benneth Ben-Azu, 2025. Preventive antioxidant strategies to reduce the effects of phthalate exposure on reproductive health. Discover Environ., 3.
- Obukohwo, O.M., P.E. Ohwin, R.A. Rume, O.G. Temitope, O.A. Oreoluwa and A.J. Motunrayo, 2024. Causes of chromosome breakage and mis-segregation affecting pregnancy and newborn health: An insight into developing reproductive health preventive strategies. OBM Genet., 8.
- Maas, J., R.A. Verheij, P.P. Groenewegen, S. de Vries and P. Spreeuwenberg, 2006. Green space, urbanity, and health: How strong is the relation? J. Epidemiol. Community Health, 60: 587-592.
- Harris, J.A., M.N. Menke, J.K. Haefner, M.H. Moniz and C.R. Perumalswami, 2017. Geographic access to assisted reproductive technology health care in the United States: A population-based cross-sectional study. Fertil. Sterility, 107: 1023-1027.
- Komorowski, A.S. and T. Jain, 2022. A review of disparities in access to infertility care and treatment outcomes among Hispanic women. Reprod. Biol. Endocrinol., 20.
- Sutton, M.Y., N.F. Anachebe, R. Lee and H. Skanes, 2021. Racial and ethnic disparities in reproductive health services and outcomes, 2020. Obstet. Gynecology, 137: 225-233.
- Alexander, M., 2021. Rural health inequity and the air ambulance abyss: Time to try a coordinated, all-payer system. Wyoming Law Rev., 21.
- Selvarajah, S., S.C. Maioli, T.A. Deivanayagam, P. de Morais Sato and D. Devakumar et al., 2022. Racism, xenophobia, and discrimination: Mapping pathways to health outcomes. Lancet, 400: 2109-2124.
- Schmeer, K.K. and J. Tarrence, 2018. Racial-ethnic disparities in inflammation: Evidence of weathering in childhood? J. Health Social Behav., 59: 411-428.
- Pearl, M., J. Ahern, A. Hubbard, B. Laraia, B.P. Shrimali, V. Poon and M. Kharrazi, 2018. Life-course neighbourhood opportunity and racial-ethnic disparities in risk of preterm birth. Paediatric Perinatal Epidemiol., 32: 412-419.
- Paradies, Y., J. Ben, N. Denson, A. Elias and N. Priest et al., 2015. Racism as a determinant of health: A systematic review and meta-analysis. PLoS ONE, 10.
- Bailey, Z.D., N. Krieger, M. Agénor, J. Graves, N. Linos and M.T. Bassett, 2017. Structural racism and health inequities in the USA: Evidence and interventions. Lancet, 389: 1453-1463.
- Schwarzer, R. and A. Leppin, 1991. Social support and health: A theoretical and empirical overview. J. Social Pers. Relat., 8: 99-127.
- Leigh, B. and J. Milgrom, 2008. Risk factors for antenatal depression, postnatal depression and parenting stress. BMC Psychiatry, 8.
- Hatef, E., J.P. Weiner and H. Kharrazi, 2019. A public health perspective on using electronic health records to address social determinants of health: The potential for a national system of local community health records in the United States. Int. J. Med. Inf., 124: 86-89.
- Lines, L.M., M.C. Long, S. Zangeneh, K. dePriest, J. Piontak, J. Humphrey and S. Subramanian, 2023. Composite indices of social determinants of health: Overview, measurement gaps, and research priorities for health equity. Popul. Health Manage., 26: 332-340.
- Chen, M., X. Tan and R. Padman, 2020. Social determinants of health in electronic health records and their impact on analysis and risk prediction: A systematic review. J. Am. Med. Inf. Assoc., 27: 1764-1773.
- Zhang, Y., J. Li, J. Yu, R.T. Braun and L.P. Casalino, 2021. Social determinants of health and geographic variation in medicare per beneficiary spending. JAMA Netw. Open, 4.
- Cantor, M.N. and L. Thorpe, 2018. Integrating data on social determinants of health into electronic health records. Health Aff., 37: 585-590.
- Delanerolle, G., A. Sivakumar, M. Haddadi, O. Kurmi and P. Phiri et al., 2025. Mind the women’s health data gap: A critical factor for global health equity. Preprints.
- Merali, I., 2000. Advancing women's reproductive and sexual health rights: Using the International Human Rights system. Dev. Pract., 10: 609-624.
- Darity, W., 2005. Stratification economics: The role of intergroup inequality. J. Econ. Finance, 29: 144-153.
- Giansanti, D., 2022. Artificial intelligence in public health: Current trends and future possibilities. Int. J. Environ. Res. Public Health, 19.
- Boulos, M.N.K., G. Peng and T. VoPham, 2019. An overview of GeoAI applications in health and healthcare. Int. J. Health Geographics, 18.
- Lauriola, P., H. Crabbe, B. Behbod, F. Yip and S. Medina et al., 2020. Advancing global health through environmental and public health tracking. Int. J. Environ. Res. Public Health, 17.
- Berdahl, C.T., L. Baker, S. Mann, O. Osoba and F. Girosi, 2023. Strategies to improve the impact of artificial intelligence on health equity: Scoping review. JMIR AI, 2.
- Delehant, S., J.R. Hatton, H. Sudhalkar and E.A. Scruth, 2024. Social determinants of health: An ethical approach. Clin. Nurse Specialist, 38: 65-68.
- Braveman, P., 2006. Health disparities and health equity: Concepts and measurement. Annu. Rev. Public Health, 27: 167-194.
- Beroukhim, G., J. Mahabamunuge and L. Pal, 2022. Racial disparities in access to reproductive health and fertility care in the United States. Curr. Opin. Obstet. Gynecology, 34: 138-146.
- Langa, N., K.F. Anderson, Z.O. Tuthill, A. Milazzo and M. Sampson et al., 2025. Intersecting social inequalities in prenatal and postnatal care: Examining race, ethnicity, socioeconomic status, and geographic location. Social Sci. Med., 384.
- Terhune, E.A., M.B. Dagne, C. Piper, A.B. Pizarro and M. Barsoum et al., 2024. Paper 3: A systematic review of definitions for “racial health equity” and related terms within health-related articles. J. Clin. Epidemiol., 176.
- Crenshaw, K., 1989. Demarginalizing the intersection of race and sex: A black feminist critique of antidiscrimination doctrine, feminist theory and antiracist politics. Univ. Chicago Legal Forum, 1989.
- Bowleg, L., 2012. The problem with the phrase women and minorities: Intersectionality-an important theoretical framework for public health. Am. J. Public Health, 102: 1267-1273.
- Bowleg, L., 2021. Evolving intersectionality within public health: From analysis to action. Am. J. Public Health, 111: 88-90.
- Ross, L., L. Roberts, E. Derkas, W. Peoples and P. Bridgewater, 2017. Radical Reproductive Justice: Foundation, Theory, Practice, Critique. The Feminist Press, New York, ISBN: 9781936932047, Pages: 500.
- Sigle, W., D.M. Nunes, L. Sochas, J. Chanfreau, S. Suh and K. Wilson, 2025. What reproductive justice brings to and requires of the feminist economics project. Feminist Econ., 31: 143-191.
- Williams, R.L., C. Romney, M. Kano, R. Wright and B. Skipper et al., 2015. Racial, gender, and socioeconomic status bias in senior medical student clinical decision-making: A national survey. J. Gen. Int. Med., 30: 758-767.
- Black, L.L., R. Johnson and L. vanHoose, 2015. The relationship between perceived racism/discrimination and health among black American women: A review of the literature from 2003 to 2013. J. Racial Ethnic Health Disparities, 2: 11-20.
- Lee, J., S. Kim and S.H. Nam, 2025. “Living with Silence and Shame”: A meta-synthesis of women’s lived experiences of infertility-related stigma. Int. J. Women's Health, 17: 2699-2713.
- Frieden, T.R., 2010. A framework for public health action: The health impact pyramid. Am. J. Public Health, 100: 590-595.
- van Daalen, K.R., S. Dada, R. James, H.C. Ashworth and P. Khorsand et al., 2022. Impact of conditional and unconditional cash transfers on health outcomes and use of health services in humanitarian settings: A mixed-methods systematic review. BMJ Global Health, 7.
- Ferguson, L., D. Tarantola, M. Hoffmann and S. Gruskin, 2017. Non-communicable diseases and human rights: Global synergies, gaps and opportunities. Global Public Health, 12: 1200-1227.
- Serchen, J., S. Erickson and D. Hilden, 2023. Reproductive health policy in the United States: An American College of Physicians policy brief. Ann. Intern. Med., 176: 364-366.
- Hoover, E., 2018. Environmental reproductive justice: Intersections in an American Indian community impacted by environmental contamination. Environ. Sociol., 4: 8-21.
- Cannon, J.S., M.R. Kilburn, L.A. Karoly, T. Mattox, A.N. Muchow and M. Buenaventura, 2018. Investing Early: Taking Stock of Outcomes and Economic Returns from Early Childhood Programs. RAND Corporation, Santa Monica, California, ISBN: 978-0-8330-9920-4, Pages: 286.
- Krieger, N., 2000. Discrimination and Health. In: Social Epidemiology, Berkman, L.F. and I. Kawachi (Eds.), Oxford University Press, New York, USA, ISBN: 9780197737941, pp: 36-75.
- Williams, D.R. and S.A. Mohammed, 2009. Discrimination and racial disparities in health: Evidence and needed research. J. Behav. Med., 32: 20-47.
- Desai, S., M. Misra, A. Das, R.J. Singh and M. Sehgal et al., 2020. Community interventions with women’s groups to improve women’s and children’s health in India: A mixed-methods systematic review of effects, enablers and barriers. BMJ Global Health, 5.
- Ruhm, C.J., 1998. The economic consequences of parental leave mandates: Lessons from Europe. Q. J. Econ., 113: 285-317.
- Tsai, Z., N. Shah, U. Tahir, N. Mortaji, S. Owais, M. Perreault and R.J. van Lieshout, 2023. Dietary interventions for perinatal depression and anxiety: A systematic review and meta-analysis of randomized controlled trials. Am. J. Clin. Nutr., 117: 1130-1142.
- Kindig, D. and G. Stoddart, 2003. What is population health? Am. J. Public Health, 93: 380-383.
- Pennel, C.L., K.R. McLeroy, J.N. Burdine, D. Matarrita-Cascante and J. Wang, 2016. Community health needs assessment: Potential for population health improvement. Popul. Health Manage., 19: 178-186.
- Vella, E., V.M. White and P. Livingston, 2022. Does cultural competence training for health professionals impact culturally and linguistically diverse patient outcomes? A systematic review of the literature. Nurse Educ. Today, 118.
- Sobczak, A., L. Taylor, S. Solomon, J. Ho and S. Kemper et al., 2023. The effect of doulas on maternal and birth outcomes: A scoping review. Cureus, 15.
- Elwyn, G., D. Frosch, R. Thomson, N. Joseph-Williams and Amy Lloyd et al., 2012. Shared decision making: A model for clinical practice. J. Gen. Intern. Med., 27: 1361-1367.
How to Cite this paper?
APA-7 Style
Oyovwi,
M.O., Oluwafemi,
E.J., Olasunkanmi,
O.J. (2026). Social Determinants of Neuro-Reproductive Health: Bridging Data Management, Equity, and Policy Intervention: Systematic Review. Trends in Social Sciences, 2(1), 24-34. https://doi.org/10.21124/tss.2026.24.34
ACS Style
Oyovwi,
M.O.; Oluwafemi,
E.J.; Olasunkanmi,
O.J. Social Determinants of Neuro-Reproductive Health: Bridging Data Management, Equity, and Policy Intervention: Systematic Review. Trends Social Sci 2026, 2, 24-34. https://doi.org/10.21124/tss.2026.24.34
AMA Style
Oyovwi
MO, Oluwafemi
EJ, Olasunkanmi
OJ. Social Determinants of Neuro-Reproductive Health: Bridging Data Management, Equity, and Policy Intervention: Systematic Review. Trends in Social Sciences. 2026; 2(1): 24-34. https://doi.org/10.21124/tss.2026.24.34
Chicago/Turabian Style
Oyovwi, Mega, Obukohwo, Egbinade Joshua Oluwafemi, and Owoeye James Olasunkanmi.
2026. "Social Determinants of Neuro-Reproductive Health: Bridging Data Management, Equity, and Policy Intervention: Systematic Review" Trends in Social Sciences 2, no. 1: 24-34. https://doi.org/10.21124/tss.2026.24.34

This work is licensed under a Creative Commons Attribution 4.0 International License.




